EBOLA
The Ebola virus has been around for quite some time and in fact first appeared in 1976 in the Democratic Republic of Congo.1
The Ebola virus has been around for quite some time and in fact first appeared in 1976 in the Democratic Republic of Congo.1
However, with the invention of social media our population has 24 hour news coverage and this news can be brought to us immediately from around the world. We have recently seen an uptick in the discussion of the Ebola Virus due to the recent outbreak in Western Africa.
“The U.S. Centers for Disease Control and Prevention said that from 550,000 people to as many as 1.4 million people when under reporting of cases is taken into account could be infected by mid-January in Liberia and Sierra Leone, in a worst-case scenario generated by a computer modeling tool the agency constructed. Around 21,000 cases would occur by Sept. 30.”2
So with this information at your fingertips; are you ready for the increase in Ebola cases here in the U.S.? Is your hospital and medical staff ready to treat these types of patients? “The current outbreak in West Africa, which first started in March 2014, is the largest and most complex Ebola outbreak since the Ebola virus was first discovered in 1976.”1 This recent outbreak has developed more cases and deaths than all other previous outbreaks combined and it is only a matter of time before we have a worldwide epidemic on our hands. If the healthcare professionals and hospital administrators are not ready for this outbreak to hit our shores it could mean a catastrophic event like we have never seen; nor lived through before.
How is Ebola Transmitted?
Ebola spreads through human-to-human transmission via direct contact such as through broken skin or mucous membranes, or through the blood, body secretions, organs or other bodily fluids of infected people, and with surfaces and materials (e.g. bedding, clothing) contaminated with these fluids. Healthcare workers have frequently been infected while treating patients with suspected or confirmed Ebola Virus. This has occurred through close contact with patients when infection control precautions are not strictly practiced.
Would Your Recognize Ebola?
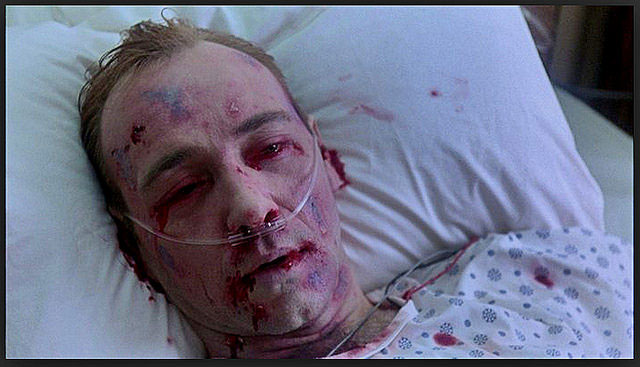
The incubation period, or the time interval from which a healthcare professional or patient has come into contact with the infectious disease and the onset of symptoms is 2 to 21 days.1 Healthcare workers and patients are not truly infectious until they develop symptoms. The first symptoms are the sudden onset of fever, fatigue, muscle pain, headache and sore throat. These are also classic signs of the influenza virus thus causing medical professionals to assume the flu and delaying the appropriate treatment. Then these initial symptoms are followed by vomiting, diarrhea, rash, symptoms of impaired kidney and liver function, and in some cases, both internal and external bleeding (e.g. oozing from the gums, blood in the stools).3 How are these patients going to get fluid replacement and hydration if they are severely dehydrated? How can we monitor their fluid status, and draw blood as safe as possible? What if there was a device invented that could be placed through a peripheral IV and left in place even after the patient went home? 6 Well, it is here; just keep reading.
How Do We Treat Ebola?
No specific vaccine or medicine (e.g., antiviral drug) has been proven to be effective against Ebola. Symptoms of Ebola are treated as they appear. The following basic interventions, when used early, can significantly improve the chances of survival:
Stay Tuned for more coming..................
How Do We Treat Ebola?
No specific vaccine or medicine (e.g., antiviral drug) has been proven to be effective against Ebola. Symptoms of Ebola are treated as they appear. The following basic interventions, when used early, can significantly improve the chances of survival:
- Providing intravenous fluids (IV)and balancing electrolytes
- Maintaining oxygen status and blood pressure
- Treating other infections if they occur
Stay Tuned for more coming..................


No comments:
Post a Comment